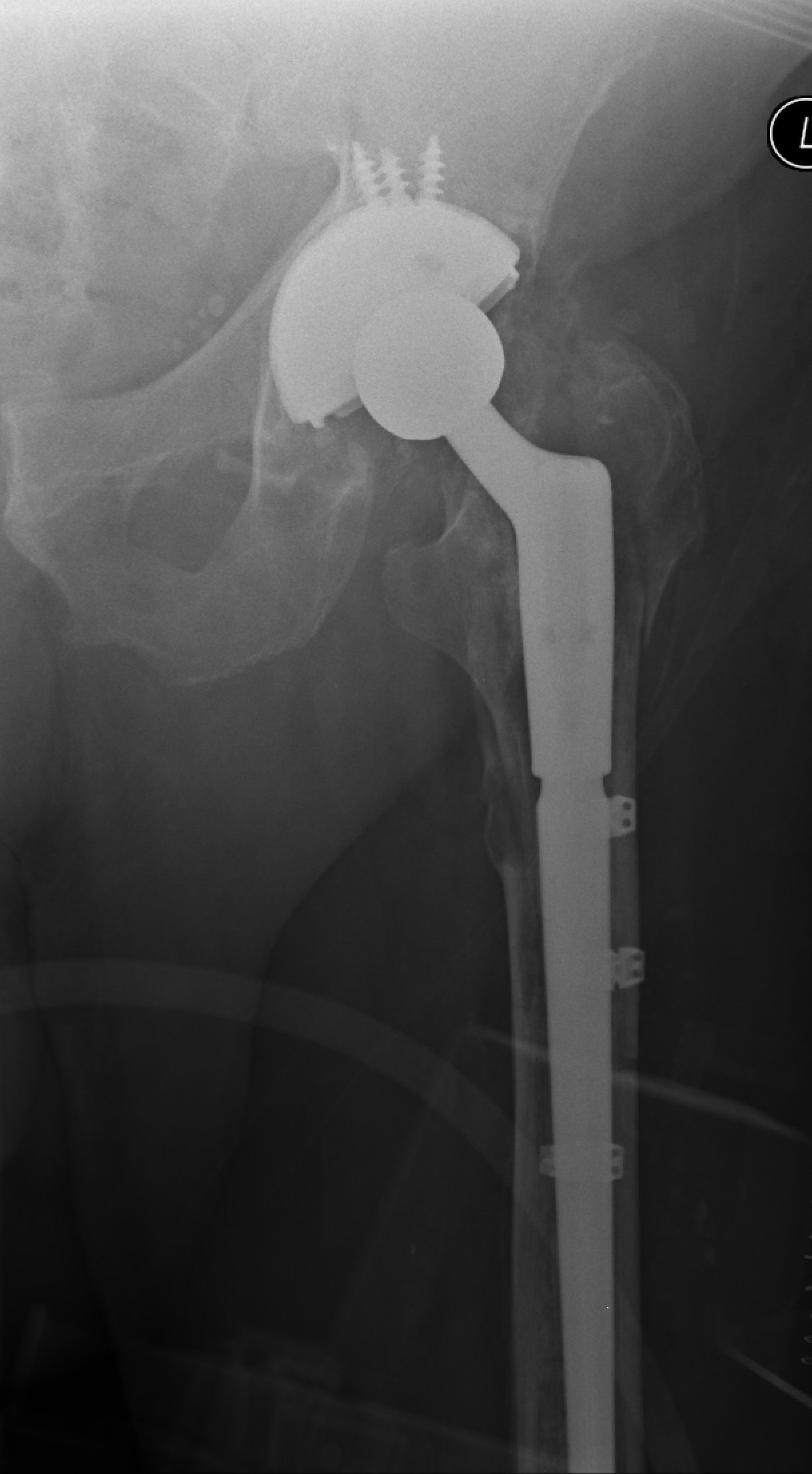
What is a revision hip replacement?
When a total hip replacement experiences mechanical or biological failure, a revision hip replacement is often required. Revision hip replacement addresses both the cause and the consequences of these failures.
It is understood that younger hip replacement patients and those with a high BMI will have more chance of requiring revision hip replacement at a later stage.
Why is a revision hip replacement needed?
A revision hip replacement is normally required to address a painful primary hip replacement as a result of worn out or loose implants, as well as infection. Patients who suffer from a hip replacement which repeatedly dislocates can also benefit from a revision hip replacement to safeguard against future dislocations. Among the groups which can be predisposed to the problem of dislocation are those who have undergone a hip replacement after having several surgeries.
What does revision hip replacement surgery involve?
Before entering the operating room, patients will have the opportunity to talk to their doctor about the procedure as a part of consent process. They will also discuss their chosen anaesthesia method with their anaesthetist.
In order to identify the problem and as a part of surgical planning the surgeon may ask for different imaging modalities. Depending on the nature of the work required, surgery involves removal of one or both components and reconstructing the hip joint using special instruments and hip implants.
In some cases, a constrained socket is used in order to secure the ball of the hip, and artificial bone substitutes or bone graft is occasionally used to address the bone loss by the surgeon. Typically, the revision hip replacement procedure involves complex surgery and takes longer than a primary total hip replacement with increased risks of complications.
Recovery time
Patients can usually resume their normal lifestyle after a 6-12week recovery period following a revision hip replacement. A course of physical therapy will be tailored by a physiotherapist to the individual patient, with the aim of strengthening the hip muscle and improving range of movement. They will also recommend different positions which are advantageous in avoiding hip dislocation in the future. Immediately following the procedure, a walking frame is typically needed, and this is replaced by crutches in the days that follow. In order to avoid problems such as deep vein thrombosis, it is recommended that mobility is returned to as swiftly as is possible.